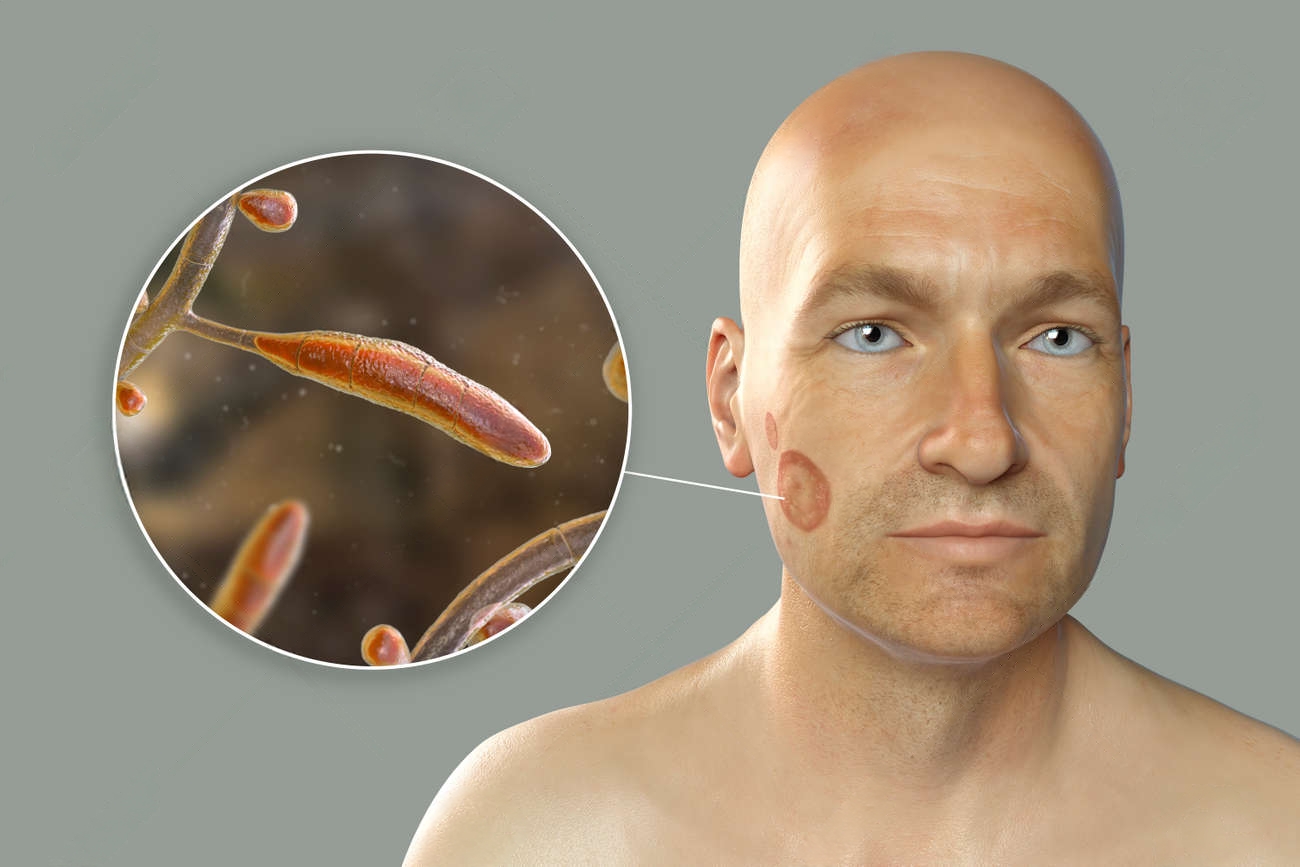
Beyond Ringworm: Understanding the Growing Fungus Health Risk
When we think of fungal infections, common ailments like athlete's foot or ringworm often come to mind. While these are prevalent, the landscape of fungal diseases is rapidly evolving, presenting an increasingly complex and concerning fungus health risk that extends far beyond the familiar. From drug-resistant strains to fungi expanding into new geographical territories, a quiet crisis is brewing, demanding our attention and a deeper understanding of how these microscopic organisms interact with our interconnected world.
The rise of emerging fungal pathogens isn't just a medical curiosity; it's a significant public health challenge influenced by environmental shifts, global travel, and even our agricultural practices. This article delves into these emerging threats, exploring the intricate ways fungi spread and highlighting the proactive measures needed to mitigate their impact on human, animal, and environmental health.
The One Health Approach: Connecting Fungi, Humans, and Animals
Understanding the modern fungus health risk requires adopting a "One Health" perspective. This crucial framework recognizes that the health of people, animals, and our shared environment are inextricably linked. Fungi, being ubiquitous in nature, perfectly illustrate this interconnectedness. They don't respect species boundaries, readily moving between hosts and thriving in various environmental niches.
Many fungal diseases are zoonotic, meaning they can spread directly between animals and people. Ringworm, for instance, is a classic example often shared between pets and their human companions. Another increasingly significant zoonotic threat is sporotrichosis, particularly the severe form caused by Sporothrix brasiliensis, which has seen a rapid expansion in South America, primarily spreading from infected cats to humans. The close contact we share with pets and livestock creates pathways for transmission that are often overlooked until an outbreak occurs.
Beyond direct zoonotic spread, fungi can also cause illness in both humans and animals without direct transmission between them. Histoplasmosis, for example, is contracted by inhaling spores found in soil contaminated with bird or bat droppings. Both people and animals can fall ill from the same environmental source, underscoring how shared environments pose a shared fungus health risk. This nuanced interplay necessitates a holistic approach to surveillance, prevention, and treatment.
Beyond the Familiar: Unmasking Emerging Fungal Threats
While common fungal infections are usually treatable, new and more aggressive strains are emerging, challenging conventional medicine and posing a serious fungus health risk. One alarming development is the spread of severe, antifungal-resistant ringworm caused by Trichophyton (T.) indotineae. This strain, initially prevalent in South Asia, has now been detected in individuals in the United States. What makes T. indotineae particularly concerning is its resistance to standard antifungal treatments, making infections persistent and difficult to eradicate. While animal infections with this specific strain haven't been reported in the U.S. yet, health officials remain highly vigilant due to the potential for cross-species transmission, as seen in the Indian subcontinent.
Other fungi, historically confined to specific regions, are now expanding their geographical range. Climate change is a key driver here, creating new hospitable environments for fungi that cause diseases like blastomycosis, Valley Fever (coccidioidomycosis), histoplasmosis, and infections from Cryptococcus gattii. As temperatures warm, these fungi can thrive in previously unsuitable areas, exposing new populations to infection risks. For example, Valley Fever, once largely restricted to the southwestern U.S., is now being identified in states further north and east, expanding the disease's footprint and increasing regional fungus health risk.
Moreover, the increased frequency of extreme weather events, such as severe flooding and high winds, exacerbates exposure. Flooding can lead to rampant mold growth in homes and buildings, increasing inhalation risks. High winds can carry fungal spores over vast distances, disseminating pathogens far from their original habitat and contributing to unexpected outbreaks.
Environmental Factors: Climate Change, Antifungal Resistance, & Amplified Risks
The interconnectedness of our world means that seemingly unrelated factors can significantly amplify the fungus health risk. Two primary drivers in this regard are climate change and the widespread use of antifungals and fungicides.
Climate Change and Fungal Expansion
As mentioned, changing global climates play a pivotal role in the emergence and spread of fungal diseases. Warmer temperatures extend the growing seasons and geographical reach of many pathogenic fungi. This means fungi adapted to warmer climates can survive and reproduce in new regions, increasing the likelihood of human and animal exposure. For instance, fungi like Coccidioides (Valley Fever) and Blastomyces thrive in specific soil conditions that are shifting with climate patterns.
Additionally, altered precipitation patterns, including both prolonged droughts and intense rainfall, can impact fungal spore dispersal. Droughts can lead to drier, dustier conditions where spores are easily aerosolized, while heavy rains and subsequent flooding create ideal conditions for mold growth, both indoors and outdoors. These environmental shifts mean that populations previously unaffected by certain fungal infections are now at risk, often without the necessary awareness or diagnostic capabilities.
The Looming Threat of Antifungal Resistance
Perhaps one of the most insidious emerging fungus health risk factors is antifungal resistance. Just like bacteria can become resistant to antibiotics, fungi can develop resistance to antifungal medications. This resistance isn't solely driven by overuse in human medicine; it's a complex issue with roots in agriculture and industry. Many fungicides used to protect crops and in industrial applications share structural similarities with antifungal medications used in human and animal medicine (e.g., azoles).
When fungi in the environment are repeatedly exposed to these agricultural fungicides, they can develop resistance mechanisms. This resistance can then transfer to fungi that later infect humans or animals, rendering our medical treatments ineffective. A prime example is azole-resistant aspergillosis, where environmental exposure to azole fungicides in agriculture is believed to contribute to the rise of drug-resistant Aspergillus infections in humans. This highlights a critical "One Health" blind spot: actions taken in one sector (agriculture) can have profound, unintended consequences for human and animal health, escalating the overall fungus health risk. To learn more about how these factors intersect, read our detailed article: Climate & Fungicide Use: Unpacking Rising Fungal Infection Risks.
Protecting Yourself and Your Community: Practical Strategies
Given the growing fungus health risk, proactive measures are essential. Individual actions, combined with broader public health strategies, can make a significant difference:
- Environmental Awareness: Be mindful of activities that stir up dust in areas known for endemic fungi (e.g., digging, construction in specific regions for Valley Fever). When possible, use masks in dusty environments.
- Pet Care & Hygiene: Regularly check pets for skin lesions, hair loss, or unusual behavior that might indicate a fungal infection. Practice good hygiene after handling pets and wear gloves when cleaning litter boxes or dealing with potentially contaminated soil.
- Post-Flood Precautions: If your home experiences flooding, address mold growth promptly and safely. Wear appropriate personal protective equipment (PPE) like N95 masks, gloves, and eye protection during cleanup. Ensure thorough drying and professional remediation if needed.
- Recognize Symptoms: Be aware of the symptoms of common and emerging fungal infections, which can often mimic bacterial or viral illnesses. Persistent respiratory symptoms, skin rashes, or unusual lesions, especially after potential exposure, warrant a medical consultation.
- Advocate for One Health: Support policies and research that integrate human, animal, and environmental health considerations, particularly regarding antimicrobial stewardship and climate change mitigation.
Conclusion
The threat posed by emerging fungal diseases is a complex, multi-faceted fungus health risk that demands our attention. From drug-resistant ringworm to fungi expanding their geographical reach due to climate change and the pervasive issue of antifungal resistance, these microscopic organisms are quietly shaping a new chapter in global health. Recognizing the interconnectedness of human, animal, and environmental health through a One Health lens is no longer optional but imperative. By understanding how fungi spread, being vigilant about environmental changes, and practicing informed prevention, we can collectively work towards mitigating this growing threat and safeguarding our future health.